New Patient Registration
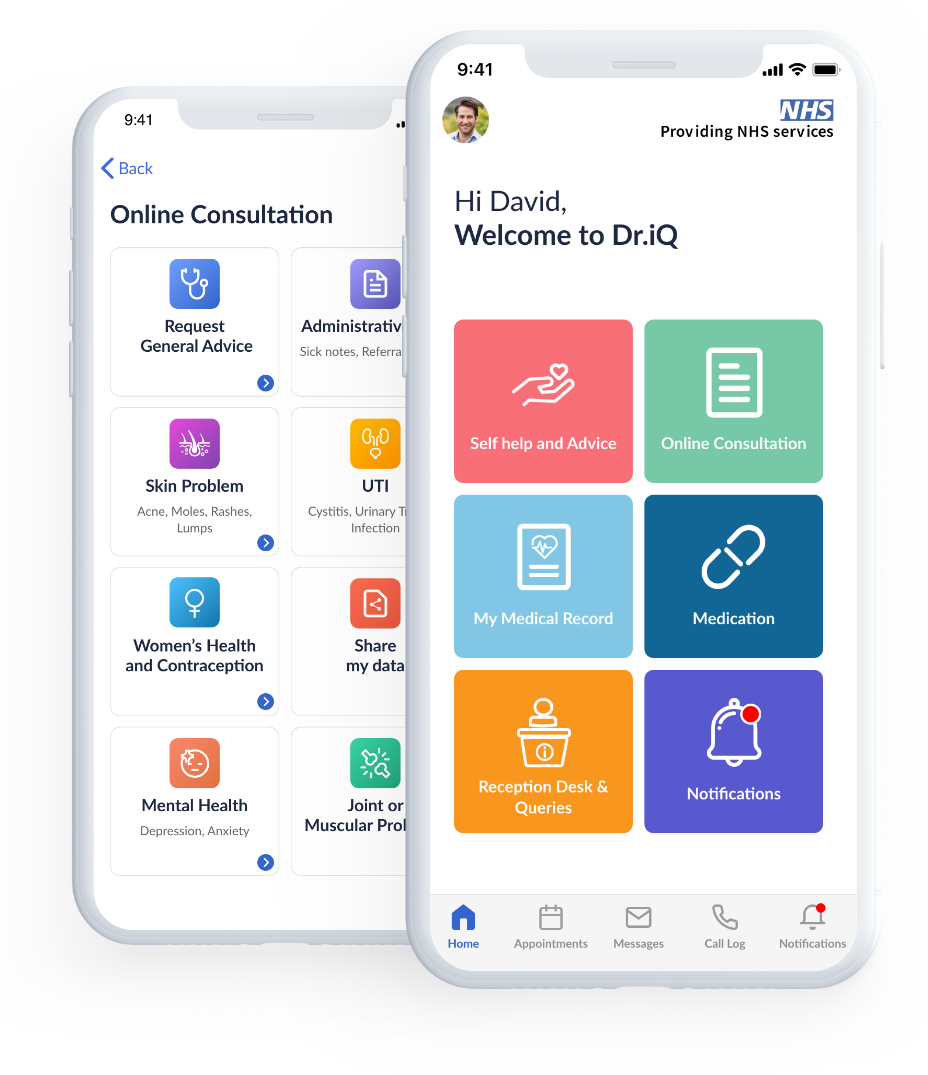
We welcome new patients. You can register via Dr. iQ or on our website.
Safe Surgeries
We are a Safe Surgery – everyone in our community is welcome at our practice.
Self Care
We are committed to empowering our patients with access to self care resources. This helps to keep you well and to find local services at your convenience.
Appointments
We encourage all patients who need an appointment to download our practice mobile app Dr. iQ. This is the fastest way to access the practice.
Repeat medication
If you need to order medications regularly, the quickest and easiest way is via Dr. iQ. You can collect your medication directly from your preferred pharmacy, usually on the same day.
Our Multidisciplinary
Healthcare Team
We have a range of highly skilled and qualified professionals working together with our GPs to deliver high quality support for you, our patients and carers.
Managing COVID-19
If you or someone you know is suffering or recovering from COVID-19, we have a range of useful resources that can help you to manage.
Update my details
If you move home, change your telephone number or email address, you can easily update your contact details with us.
CQC Ratings
You can see the reports or find out more information about what our CQC ratings mean for you.

You can see the reports or find out more information about what our CQC ratings mean for you.
Learn MorePractice Timings
Carpenters Practice
Carpenters Practice 236-252 High Street, Stratford, E15 2JA
Opening Times |
|
| Mon - Thur | 8:00am – 6:30pm |
| Friday | 8:00am – 6:30pm |
| Sat - Sun | Closed |
| More details | |
Church Road Practice
Church Road Practice The Centre Manor Park, 30 Church Road, Manor Park, E12 6AQ
Opening Times |
|
| Mon - Fri | 8:00am – 6:30pm |
| Friday | 8:00am – 6:30pm |
| Sat - Sun | Closed |
| More details | |
E16 Health - Albert Road
E16 Health - Albert Road 76 Albert Rd, Royal Docks, London E16 2DY
Opening Times |
|
| Mon - Fri | 8:00am – 6:30pm |
| Saturday | 9:00am – 1:00pm |
| Sunday | Closed |
| More details | |
E16 Health - Pontoon Dock
E16 Health - Pontoon Dock, Royal Wharf, North Woolwich Road, London E16 2HP
Opening Times |
|
| Mon - Fri | 8:00am – 6:30pm |
| Saturday | 9:00am – 1:00pm |
| Sunday | Closed |
| More details | |
Lucas Avenue Practice
Lucas Avenue Practice 1A Lucas Avenue, Upton Park, E13 0QP
Opening Times |
|
| Mon - Fri | 8:00am – 6:30pm |
| Saturday | 9:00am – 1:00pm |
| Sunday | Closed |
| More details | |
St Luke's Practice
St Luke's Practice 2 St Luke’s Square, Canning Town, E16 1HT
Opening Times |
|
| Mon - Thurs | 8:00am – 6:30pm |
| Friday | 8:00am – 6:30pm |
| Sat - Sun | Closed |
| More details | |